
| Bone Broken | Time for it to Heal |
Collar bone (clavicle) | 3-8 weeks |
Shoulder blade (scapula) | 6 weeks |
Ribs | 4 weeks |
Upper arm (humerus) | 4-10 weeks |
Lower arm (radius,ulna) | 6 weeks |
Wrist | 4-12 weeks |
Fingers | 4-6 weeks |
Pelvis | 4 - 6 weeks |
Upper leg (femur) | 12 weeks |
Knee (patella) | 4-6 weeks |
Lower leg (tibia,fibula) | 10-24 weeks |
Ankle | 6 weeks |
Foot | 3 - 12 weeks |
Toes | 3 weeks |
Thanks to:
http://www.doctorsecrets.com/your-bones/time-to-heal-broken-bone.htm
----------
Bone fracture
From Wikipedia, the free encyclopedia
| Bone fracture | |
|---|---|
| Classification and external resources | |
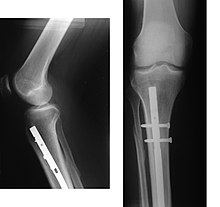
 Internal and external views of an arm with a compound fracture, both before and after surgery. | |
| ICD-10 | Sx2 (where x=0-9 depending on the location of the fracture) |
| ICD-9 | 829 |
| DiseasesDB | 4939 |
| MeSH | D050723 |
Although broken bone and bone break are common colloquialisms for a bone fracture, break is not a formal orthopedic term.
Contents[hide] |
Classification
Orthopedic
In orthopedic medicine, fractures are classified in various ways. Historically they are named after the doctor who first described the fracture conditions. However, there are more systematic classifications in place currently.All fractures can be broadly described as:
- Closed (simple) fractures are those in which the skin is intact
- Open (compound) fractures involve wounds that communicate with the fracture, or where fracture hematoma is exposed, and may thus expose bone to contamination. Open injuries carry a higher risk of infection.
- Compression fractures usually occurs in the vertebrae, for example when the front portion of a vertebra in the spine collapses due to osteoporosis (a medical condition which causes bones to become brittle and susceptible to fracture, with or without trauma).
- Complete fracture: A fracture in which bone fragments separate completely.
- Incomplete fracture: A fracture in which the bone fragments are still partially joined. In such cases, there is a crack in the osseous tissue that does not completely traverse the width of the bone.[1]
- Linear fracture: A fracture that is parallel to the bone's long axis.
- Transverse fracture: A fracture that is at a right angle to the bone's long axis.
- Oblique fracture: A fracture that is diagonal to a bone's long axis.
- Spiral fracture: A fracture where at least one part of the bone has been twisted.
- Comminuted fracture: A fracture in which the bone has broken into a number of pieces.
- Impacted fracture: A fracture caused when bone fragments are driven into each other.
Anatomical
An anatomical classification may begin with specifying the involved body part, such as the head or arm, followed with more specific localization. Fractures that have additional definition criteria than merely localization can often be classified as subtypes of fractures that merely are, such as a Holstein-Lewis fracture being a subtype of a humerus fracture. However, most typical examples in an orthopedic classification given in previous section cannot appropriately be classified into any specific part of an anatomical classification, as they may apply to multiple anatomical fracture sites.- Skull fracture
- Basilar skull fracture
- Blowout fracture - a fracture of the walls or floor of the orbit
- Mandibular fracture
- Nasal fracture
- Le Fort fracture of skull - facial fractures involving the maxillary bone and surrounding structures in a usually bilateral and either horizontal, pyramidal or transverse way.
- Spinal fracture
- Cervical fracture
- Fracture of C1, including Jefferson fracture
- Fracture of C2, including Hangman's fracture
- Flexion teardrop fracture - a fracture of the anteroinferior aspect of a cervical vertebral
- Clay-shoveler fracture - fracture through the spinous process of a vertebra occurring at any of the lower cervical or upper thoracic vertebrae
- Burst fracture - in which a vertebra breaks from a high-energy axial load
- Compression fracture - a collapse of a vertebra, often in the form of wedge fractures due to larger compression anteriorly.
- Chance fracture - compression injury to the anterior portion of a vertebral body with concomitant distraction injury to posterior elements
- Holdsworth fracture - an unstable fracture dislocation of the thoraco lumbar junction of the spine
- Cervical fracture
- Arm fracture
- Humerus fracture (fracture of upper arm)
- Supracondylar fracture
- Holstein-Lewis fracture - a fracture of the distal third of the humerus resulting in entrapment of the radial nerve.
- Forearm fracture
- Ulnar fracture
- Monteggia fracture - a fracture of the proximal third of the ulna with the dislocation of the head of the radius
- Hume fracture - a fracture of the olecranon with an associated anterior dislocation of the radial head
- Radius fracture
- Essex-Lopresti fracture - a fracture of the radial head with concomitant dislocation of the distal radio-ulnar joint with disruption of the interosseous membrane.[2]
- Distal radius fracture
- Galeazzi fracture - a fracture of the radius with dislocation of the distal radioulnar joint
- Colles' fracture - a distal fracture of the radius with dorsal (posterior) displacement of the wrist and hand
- Smith's fracture - a distal fracture of the radius with volar (ventral) displacement of the wrist and hand
- Barton's fracture - an intra-articular fracture of the distal radius with dislocation of the radiocarpal joint.
- Ulnar fracture
- Humerus fracture (fracture of upper arm)
- Hand fracture
- Scaphoid fracture
- Rolando fracture - a comminuted intra-articular fracture through the base of the first metacarpal bone
- Bennett's fracture - a fracture of the base of the first metacarpal bone which extends into the carpometacarpal (CMC) joint.[3]
- Boxer's fracture - a fracture at the neck of a metacarpal
- Pelvic fracture
- Fracture of the hip bone
- Duverney fracture - an isolated pelvic fracture involving only the iliac wing.
- Femoral fracture
- Hip fracture (anatomically a fracture of the femur bone and not the hip bone)
- Crus fracture
- Tibia fracture
- Bumper fracture - a fracture of the lateral tibial plateau caused by a forced valgus applied to the knee
- Segond fracture - an avulsion fracture of the lateral tibial condyle
- Gosselin fracture - a fractures of the tibial plafond into anterior and posterior fragments[4]
- Toddler's fracture - an undisplaced and spiral fracture of the distal third to distal half of the tibia[5]
- Fibular fracture
- Maisonneuve fracture - a spiral fracture of the proximal third of the fibula associated with a tear of the distal tibiofibular syndesmosis and the interosseous membrane.
- Le Fort fracture of ankle - a vertical fracture of the antero-medial part of the distal fibula with avulsion of the anterior tibiofibular ligament.[6]
- Bosworth fracture - a fracture with an associated fixed posterior dislocation of the proximal fibular fragment which becomes trapped behind the posterior tibial tubercle. The injury is caused by severe external rotation of the ankle.[7]
- Combined tibia and fibula fracture
- Trimalleolar fracture - involving the lateral malleolus, medial malleolus and the distal posterior aspect of the tibia
- Bimalleolar fracture - involving the lateral malleolus and the medial malleolus.
- Pott's fracture
- Tibia fracture
- Foot fracture
- Lisfranc fracture - in which one or all of the metatarsals are displaced from the tarsus[8]
- Jones fracture - a fracture of the fifth metatarsal
- March fracture - a fracture of the distal third of one of the metatarsals occurring because of recurrent stress
- Calcaneal fracture
OTA classification
The Orthopaedic Trauma Association, an association for orthopaedic surgeons, adopted and then extended the classification of Müller and the AO foundation [9] ("The Comprehensive Classification of the Long Bones") an elaborate classification system to describe the injury accurately and guide treatment.[10][11] There are five parts to the code:- Bone: The OTA classification of a fracture starts by coding for the bone involved:
- Location: a code for the part of the bone involved (e.g. shaft of the femur): proximal=1, diaphyseal=2, distal=3 (at the ankle the malleolar region is considered separately due to the pre-existing Weber classification and coded as 4[12]). Except at the proximal femur the distal and proximal regions of the bone are defined by a square that is as wide as the as the distance between the condyles. The diaphysis is considered to be the rest of the bone between these two squares.
- Type: It is important to note whether the fracture is simple or multifragmentary and whether it is closed or open: A=simple fracture, B=wedge fracture, C=complex fracture
- Group: The geometry of the fracture is also described by terms such as transverse, oblique, spiral, or segmental.
- Subgroup: Other features of the fracture are described in terms of displacement, angulation and shortening. A stable fracture is one which is likely to stay in a good (functional) position while it heals; an unstable one is likely to shorten, angulate or rotate before healing and lead to poor function in the long term.
Other classification systems
There are other systems used to classify different types of bone fractures:- "Denis classification" for spinal fractures[13]
- "Frykman classification" for forearm fractures (fractures of radius and ulna)
- "Letournel and Judet Classification" for Acetabular fractures[15]
- "Neer classification" for humerus fractures[16][17]
- "Seinsheimer's Classification" for femoral fractures[18]
Signs and symptoms
Although bone tissue itself contains no nociceptors, bone fracture is very painful for several reasons:[19]- Breaking in the continuity of the periosteum, with or without similar discontinuity in endosteum, as both contain multiple nociceptors.
- Edema of nearby soft tissues caused by bleeding of torn periosteal blood vessels evokes pressure pain.
- Muscle spasms trying to hold bone fragments in place
Pathophysiology
Main article: Bone healing
The natural process of healing a fracture starts when the injured bone and surrounding tissues bleed, forming a fracture Hematoma. The blood coagulates to form a blood clot situated between the broken fragments. Within a few days blood vessels grow into the jelly-like matrix of the blood clot. The new blood vessels bring phagocytes to the area, which gradually remove the non-viable material. The blood vessels also bring fibroblasts in the walls of the vessels and these multiply and produce collagen fibres. In this way the blood clot is replaced by a matrix of collagen. Collagen's rubbery consistency allows bone fragments to move only a small amount unless severe or persistent force is applied.At this stage, some of the fibroblasts begin to lay down bone matrix (calcium hydroxyapatite) in the form of insoluble crystals. This mineralization of the collagen matrix stiffens it and transforms it into bone. In fact, bone is a mineralized collagen matrix; if the mineral is dissolved out of bone, it becomes rubbery. Healing bone callus is on average sufficiently mineralized to show up on X-ray within 6 weeks in adults and less in children. This initial "woven" bone does not have the strong mechanical properties of mature bone. By a process of remodeling, the woven bone is replaced by mature "lamellar" bone. The whole process can take up to 18 months, but in adults the strength of the healing bone is usually 80% of normal by 3 months after the injury.
Several factors can help or hinder the bone healing process. For example, any form of nicotine hinders the process of bone healing, and adequate nutrition (including calcium intake) will help the bone healing process. Weight-bearing stress on bone, after the bone has healed sufficiently to bear the weight, also builds bone strength. Although there are theoretical concerns about NSAIDs slowing the rate of healing, there is not enough evidence to warrant withholding the use of this type analgesic in simple fractures.[20]
Effects of nicotine
Smokers generally have lower bone density than non-smokers, so have a much higher risk of fractures. There is also evidence that smoking delays bone healing. Some research indicates, for example, that it delays tibial shaft fracture healing from a median healing time of 136 to a median healing time of 269 days[21]. This means that the fracture healing time was approximately doubled in smokers. Although some other studies show less extreme effects, it is still shown that smoking delays fracture healing.Diagnosis
A bone fracture can be diagnosed clinically based on the history given and the physical examination performed. Imaging by X-ray is often performed to view the bone suspected of being fractured. In situations where x-ray alone is insufficient, a computed tomograph (CT scan) may be performed.Treatment
Treatment of bone fractures are broadly classified as surgical or conservative, the latter basically referring to any non-surgical procedure, such as pain management, immobilization or other non-surgical stabilization. A similar classification is open versus closed treatment, in which open treatment refers to any treatment in which the fracture site is surgically opened, regardless of whether the fracture itself is an open or closed fracture.Pain management
In arm fractures in children, ibuprofen has been found to be equally effective as the combination of acetaminophen and codeine.[22][edit] Immobilization
Since bone healing is a natural process which will most often occur, fracture treatment aims to ensure the best possible function of the injured part after healing. Bone fractures are typically treated by restoring the fractured pieces of bone to their natural positions (if necessary), and maintaining those positions while the bone heals. Often, aligning the bone, called reduction, in good position and verifying the improved alignment with an X-ray is all that is needed. This process is extremely painful without anesthesia, about as painful as breaking the bone itself. To this end, a fractured limb is usually immobilized with a plaster or fiberglass cast or splint which holds the bones in position and immobilizes the joints above and below the fracture. When the initial post-fracture edema or swelling goes down, the fracture may be placed in a removable brace or orthosis. If being treated with surgery, surgical nails, screws, plates and wires are used to hold the fractured bone together more directly. Alternatively, fractured bones may be treated by the Ilizarov method which is a form of external fixator.Occasionally smaller bones, such as phalanges of the toes and fingers, may be treated without the cast, by buddy wrapping them, which serves a similar function to making a cast. By allowing only limited movement, fixation helps preserve anatomical alignment while enabling callus formation, towards the target of achieving union.
Splinting results in the same outcome as casting in children who have a distal radius fracture with little shifting.[23]
Surgery
Surgical methods of treating fractures have their own risks and benefits, but usually surgery is done only if conservative treatment has failed or is very likely to fail. With some fractures such as hip fractures (usually caused by osteoporosis or osteogenesis Imperfecta), surgery is offered routinely, because the complications of non-operative treatment include deep vein thrombosis (DVT) and pulmonary embolism, which are more dangerous than surgery. When a joint surface is damaged by a fracture, surgery is also commonly recommended to make an accurate anatomical reduction and restore the smoothness of the joint.Infection is especially dangerous in bones, due to the recrudescent nature of bone infections. Bone tissue is predominantly extracellular matrix, rather than living cells, and the few blood vessels needed to support this low metabolism are only able to bring a limited number of immune cells to an injury to fight infection. For this reason, open fractures and osteotomies call for very careful antiseptic procedures and prophylactic antibiotics.
Occasionally bone grafting is used to treat a fracture.
Sometimes bones are reinforced with metal. These implants must be designed and installed with care. Stress shielding occurs when plates or screws carry too large of a portion of the bone's load, causing atrophy. This problem is reduced, but not eliminated, by the use of low-modulus materials, including titanium and its alloys. The heat generated by the friction of installing hardware can easily accumulate and damage bone tissue, reducing the strength of the connections. If dissimilar metals are installed in contact with one another (i.e., a titanium plate with cobalt-chromium alloy or stainless steel screws), galvanic corrosion will result. The metal ions produced can damage the bone locally and may cause systemic effects as well.
Electrical bone growth stimulation or osteostimulation has been attempted to speed or improve bone healing. Results however do not support its effectiveness.[24]
Complications
Some fractures can lead to serious complications including a condition known as compartment syndrome. If not treated, compartment syndrome can result in amputation of the affected limb. Other complications may include non-union, where the fractured bone fails to heal or mal-union, where the fractured bone heals in a deformed manner.In children
Main article: Child bone fracture
In children, whose bones are still developing, there are risks of either a growth plate injury or a greenstick fracture.- A greenstick fracture occurs due to mechanical failure on the tension side. That is, since the bone is not as brittle as it would be in an adult, it does not completely fracture, but rather exhibits bowing without complete disruption of the bone's cortex in the surface opposite the applied force.
- Growth plate injuries, as in Salter-Harris fractures, require careful treatment and accurate reduction to make sure that the bone continues to grow normally.
- Plastic deformation of the bone, in which the bone permanently bends but does not break, is also possible in children. These injuries may require an osteotomy (bone cut) to realign the bone if it is fixed and cannot be realigned by closed methods.
- Certain fractures are known to occur mainly in the pediatric age group, such as fracture of the clavicle & supracondylar fracture of the humerus.
See also
- Distraction osteogenesis
- Rickets
- Catagmatic
- H. Winnett Orr, US Army surgeon who developed Orthopedic plaster casts
References
- ^ TheFreeDictionary > incomplete fracture Citying: Mosby's Medical Dictionary, 8th edition. © 2009
- ^ Essex Lopresti fracture at Wheeless' Textbook of Orthopaedics online
- ^ Bennett's fracture-subluxation at GPnotebook
- ^ Hunter, Tim B; Leonard F Peltier, Pamela J Lund (May 2000). "Musculoskeletal Eponyms: Who Are Those Guys?". RadioGraphics 20 (3): 819–836. Retrieved 2009-10-17.
- ^ Mellick LB, Milker L, Egsieker E (October 1999). "Childhood accidental spiral tibial (CAST) fractures". Pediatr Emerg Care 15 (5): 307–9. doi:10.1097/00006565-199910000-00001. PMID 10532655.
- ^ Tim B Hunter, Leonard F Peltier, Pamela J Lund (2000). "Musculoskeletal Eponyms: Who Are Those Guys?". RadioGraphics 20: 829. Retrieved 2009-11-13.
- ^ Perry, CR; Rice S, Rao A, Burdge R. (Oct 1983). "Posterior fracture-dislocation of the distal part of the fibula. Mechanism and staging of injury.". J Bone Joint Surg Am. 65 (8): 1149–57. PMID 6630259. Retrieved 2009-10-10.
- ^ TheFreeDictionary > Lisfranc's fracture Citing: Mosby's Medical Dictionary, 8th edition. Copyright 2009
- ^ http://www.ota.org/compendium/2007JOTFractureCompNew/97042.2Introduction%20S1-S6.pdf
- ^ "Fracture and dislocation compendium. Orthopaedic Trauma Association Committee for Coding and Classification" (pdf). J Orthop Trauma 10 Suppl 1: v–ix, 1–154. 1996. PMID 8814583. Archived from the original on 2007-09-28. Retrieved 2007-11-28.
- ^ "Orthopaedic Trauma Association/ Committee for Coding and Classification: Fracture and Dislocation Compendium". Orthopaedic Trauma Association. Retrieved 2007-11-28.
- ^ "Proximal forearm - AO Surgery Reference".
- ^ 1590689797 at GPnotebook
- ^ Rüedi, etc. all; Thomas P. Rüedi, Richard E. Buckley, Christopher G. Moran (2007). AO principles of fracture management, Volume 1. Thieme. p. Page 96. ISBN 3131174420.
- ^ "Fractures of the Acetabulum".
- ^ Mourad L (1997). "Neer classification of fractures of the proximal humerus". Orthop Nurs 16 (2): 76. PMID 9155417.
- ^ "eMedicine - Proximal Humerus Fractures: Article by Mark Frankle, MD". Retrieved 2007-12-15.
- ^ "Seinsheimer's Classification of Subtrochanteric Frxs - Wheeless' Textbook of Orthopaedics". Retrieved 2007-12-15.
- ^ MedicineNet - Fracture Medical Author: Benjamin C. Wedro, MD, FAAEM.
- ^ "BestBets: Do non-steroidal anti-inflammatory drugs cause a delay in fracture healing?".
- ^ http://www.medicine.ox.ac.uk/bandolier/booth/painpag/wisdom/NSAIbone.html
- ^ Drendel AL, Gorelick MH, Weisman SJ, Lyon R, Brousseau DC, Kim MK (October 2009). "A randomized clinical trial of ibuprofen versus acetaminophen with codeine for acute pediatric arm fracture pain". Ann Emerg Med 54 (4): 553–60. doi:10.1016/j.annemergmed.2009.06.005. PMID 19692147.
- ^ Boutis K, Willan A, Babyn P, Goeree R, Howard A (October 2010). "Cast versus splint in children with minimally angulated fractures of the distal radius: a randomized controlled trial". CMAJ 182 (14): 1507–12. doi:10.1503/cmaj.100119. PMC 2950182. PMID 20823169.
- ^ Mollon B, da Silva V, Busse JW, Einhorn TA, Bhandari M (November 2008). "Electrical stimulation for long-bone fracture-healing: a meta-analysis of randomized controlled trials". J Bone Joint Surg Am 90 (11): 2322–30. doi:10.2106/JBJS.H.00111. PMID 18978400.
External links
| Wikimedia Commons has media related to: Fractures |
- First Aid for Fractures Wildernessmanuals.com
- Fracture and Dislocation Compendium Orthopaedic Trauma Association
- Authoritative information in orthopaedic surgery American Association of Orthopedic Surgeons (AAOS)
- Radiographic Atlas of Fracture
- After the Injury Children's Hospital Of Philadelphia
http://en.wikipedia.org/wiki/Bone_fracture

No comments:
Post a Comment